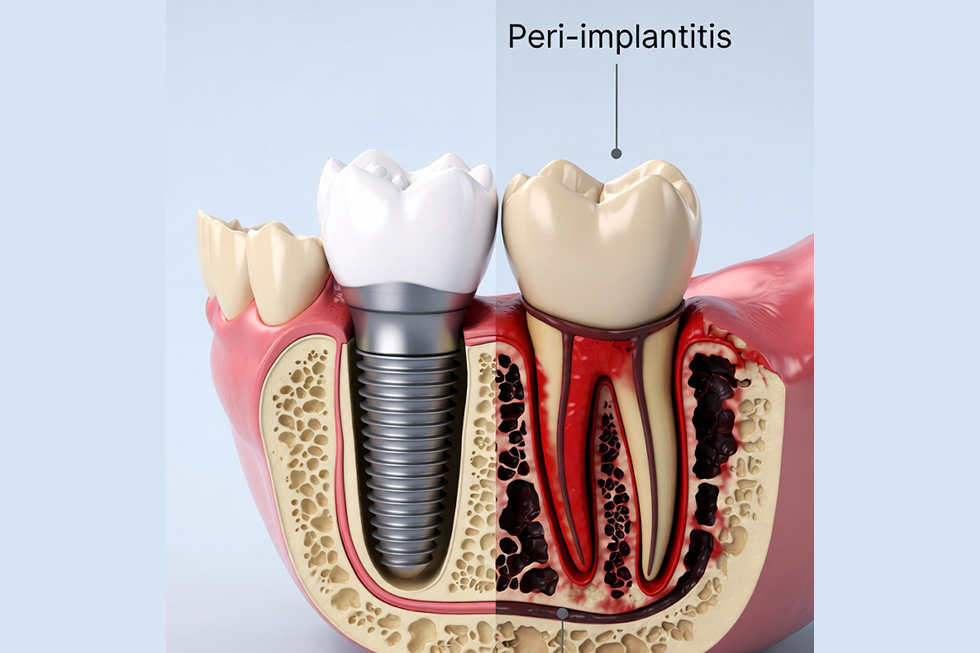
Dental implants have changed the way we replace missing teeth. They look natural, feel stable, and help preserve jaw function.
As a periodontist with decades of clinical experience, I often see patients who are surprised when problems develop around their implants. One of the most common (and often overlooked) conditions is peri-implantitis. Dr. Nooshin Ghayoumi emphasizes that early awareness can make a significant difference in long-term outcomes.
Peri-implantitis develops quietly. It may not cause pain at first, yet it can gradually damage the bone supporting the implant. If left untreated, it can lead to implant failure.
What Is Peri-Implantitis?
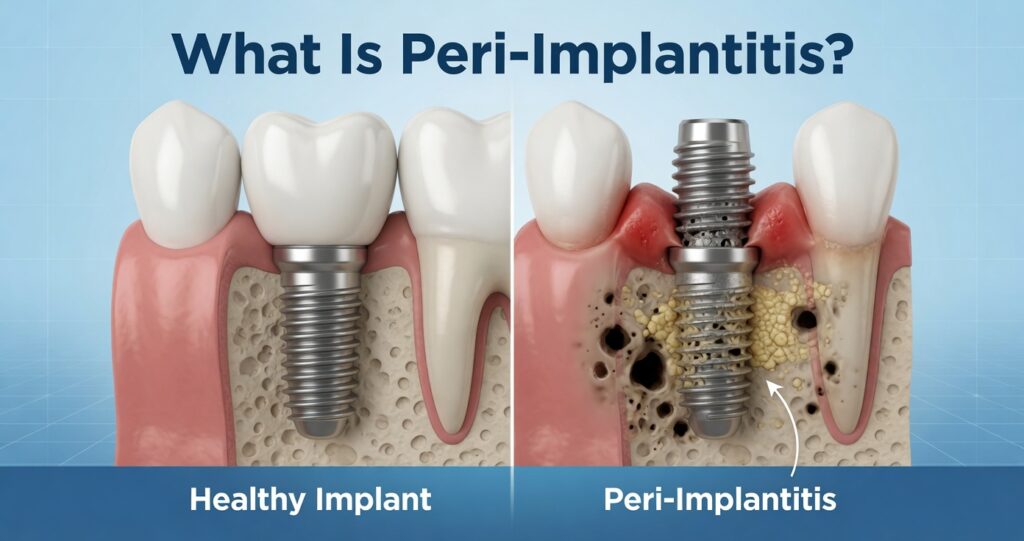
Peri-implantitis is an inflammatory condition that affects the tissues around a dental implant. It involves two main components:
- Inflammation of the gum (soft tissue)
- Progressive loss of the supporting bone
There is an earlier stage called peri-implant mucositis. At this stage, the inflammation is limited to the gums and is still reversible. Once bone loss begins, the condition progresses into peri-implantitis, which requires more advanced treatment.
Quick Comparison: Peri-Implantitis vs Gum Disease
| Feature | Gum Disease (Periodontitis) | Peri-Implantitis |
|---|---|---|
| Affected Area | Natural teeth | Dental implants |
| Cause | Bacterial plaque buildup | Bacterial infection around implant |
| Supporting Structure | Periodontal ligament present | No periodontal ligament |
| Progression | Often gradual | Can progress more rapidly |
| Bone Loss | Occurs over time | Can occur faster and more aggressively |
| Early Stage | Gingivitis (reversible) | Peri-implant mucositis (reversible) |
| Advanced Stage | Periodontitis | Peri-implantitis |
| Risk Factors | Poor hygiene, smoking, genetics | Poor hygiene, smoking, history of gum disease, implant-related factors |
| Treatment | Scaling, root planing, surgery | Implant cleaning, surface decontamination, possible surgery |
Patients with a history of gum disease have a higher risk of developing peri-implantitis. This is why careful periodontal evaluation before and after implant placement remains essential for long-term success.
Why Is It Called a Silent Threat?
Many people expect pain to signal a problem. Peri-implantitis frequently breaks that expectation. In its beginning stages, symptoms stay subtle. Discomfort may be absent. Nothing obvious draws attention.
So what should you look for?
- Slight bleeding when brushing
- Mild swelling around the implant
- A persistent bad taste
These signs are easy to ignore. Over time, the infection continues to affect the bone. By the time noticeable symptoms appear, damage may already be significant.
This is why regular check-ups matter. Early detection gives us a chance to stop the disease before it progresses.
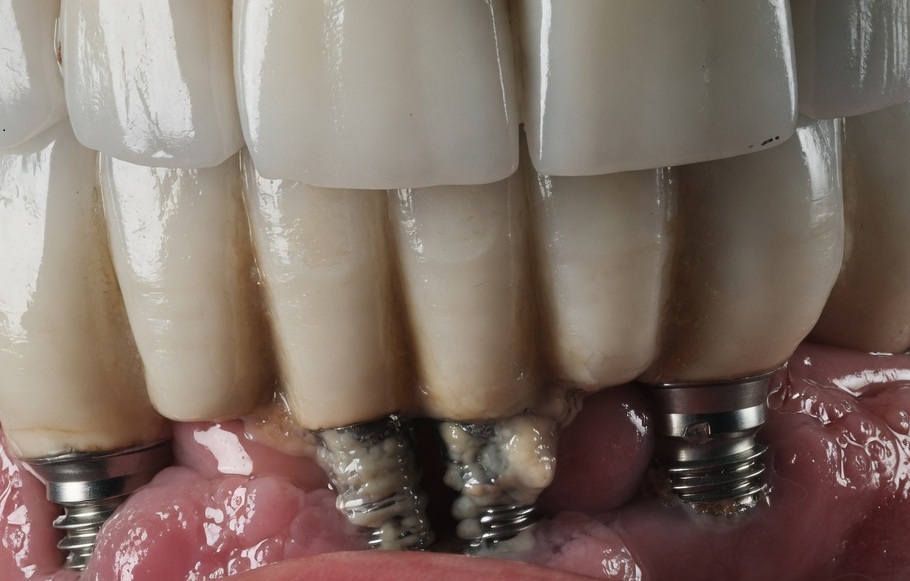
Causes and Risk Factors
Peri-implantitis does not happen randomly. Several factors increase the risk:
- Poor oral hygiene
- Smoking adds significant danger
- History of gum disease
- Irregular dental visits
- Improper implant positioning
- Excess cement around the implant
Many implants remain healthy for years. The difference often comes down to maintenance and risk factors. Patients who had gum disease in the past need closer monitoring because their tissues are more vulnerable.
Signs and Symptoms to Watch
Recognizing early signs can protect your implant. Here are the most common symptoms:
- Bleeding around the implant during brushing
- Red or swollen gums often appear
- Gum recession may expose threads or surfaces of the implant itself
- Pus or discharge
- Bad breath that does not improve
- Loosening of the implant (in advanced stages)
If you notice one or more of these signs, it is time to act. Waiting rarely improves the situation.
What Happens Without Treatment?
Peri-implantitis progresses over time. It does not remain stable.
As the condition advances:
- Bone around the implant continues to shrink
- The implant loses support
- The structure becomes unstable
In some cases, the implant may need to be removed. Patients may then require procedures such as:
- Bone grafting to rebuild lost structure
- Ridge augmentation to restore proper anatomy
- Placement of a new implant after healing
This process takes time, effort, and cost. Early treatment helps avoid these outcomes.
Treatment Options for Peri-Implantitis
The right approach depends on when we identify the condition.
Non-Surgical Treatment
In early stages, we may use:
- Professional deep cleaning around the implant
- Antimicrobial rinses or localized medications
- Improved home care routines
These steps aim to control infection and reduce inflammation.
Surgical Treatment
When bone loss has occurred, surgical care becomes necessary:
- Flap surgery to access and clean the area
- Removal of infected tissue
- Decontamination of the implant surface
- Bone grafting to rebuild support
Patients often ask: can the implant be saved?
In numerous cases the answer is yes, provided we intervene while enough healthy structure remains.
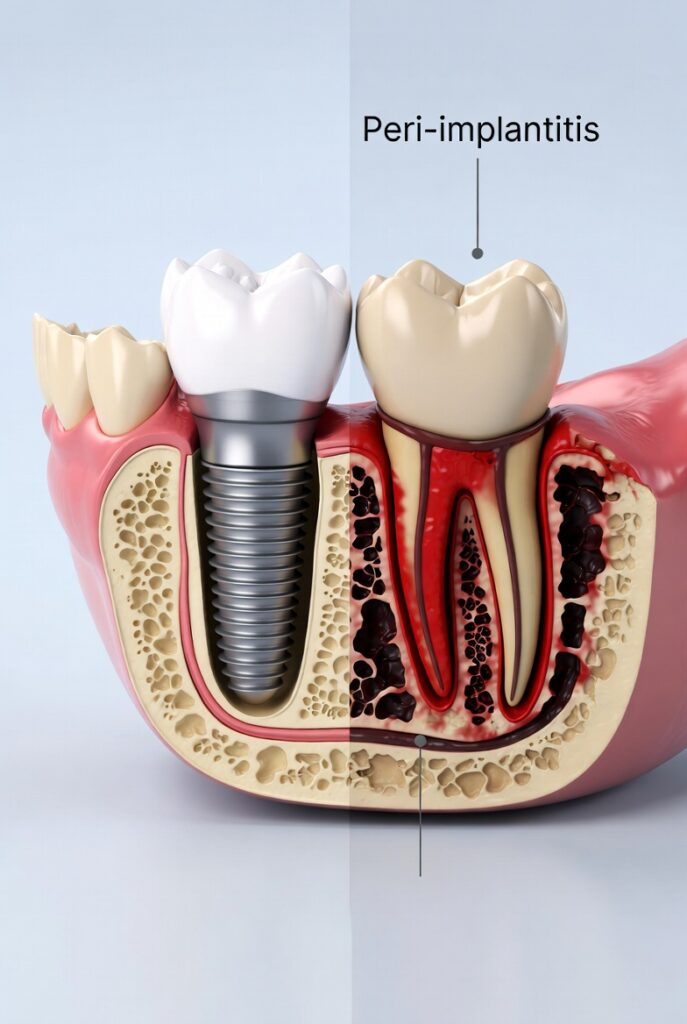
Can Peri-Implantitis Be Prevented?
Prevention offers the most effective strategy. Patients can lower their risk through consistent habits.
- Brush and floss every day using proper technique
- Choose tools specifically designed for implants
- Include routine periodontal evaluations in your calendar
- Attend scheduled professional cleanings without fail
- Avoid smoking
Conclusion
Peri-implantitis is a serious condition, yet many patients remain unaware of it until damage has already occurred. It develops quietly, progresses steadily, and can threaten the success of dental implants if ignored.
When managed properly, dental implants remain a reliable and long-lasting solution. Professional periodontal care plays a central role in keeping both the gums and supporting bone healthy. For patients seeking long-term success with their implants, guidance from experienced specialists such as Dr. Nooshin Ghayoumi can help protect both function and overall oral health.